How to Build a HIPAA-Compliant Telemedicine Platform for Peptide and Longevity Clinics
The peptide therapy market is booming, regulatory access is reopening, and clinics are scrambling to serve patients digitally. But most telehealth tools weren't built for this niche. If you're looking to build a telemedicine platform for peptide clinics or longevity practices, you're facing a unique set of challenges: complex intake workflows, 503A pharmacy integration, multi-state prescribing rules, and HIPAA compliance requirements that go well beyond a basic video call. This guide walks through exactly what it takes to build one right, from clinical features and tech stack to realistic costs and a faster alternative to traditional development.
How Do You Build a HIPAA-Compliant Telemedicine Platform for Peptide Therapy?
You start with HIPAA-ready infrastructure (encrypted storage, access controls, audit logging, BAAs with all vendors), then build the clinical workflow layer on top: async patient intake with risk stratification, e-prescribing via a Surescripts-certified integration, 503A compounding pharmacy routing, triggered video visits for flagged cases, and a secure patient portal. Traditional custom builds cost $40K–$300K+ and take 3–12 months. AI-powered healthcare app builders like Specode can compress this to weeks while giving you full code ownership.
Key Takeaways
- Peptide clinics need purpose-built telemedicine workflows, not generic telehealth tools. The core loop (async intake → risk stratification → chart review → e-prescribing → pharmacy fulfillment) is specific to this niche and drives both clinical efficiency and compliance.
- HIPAA compliance is an architecture decision, not a feature toggle. Encryption, audit logging, BAAs, and AI guardrails must be in place before any patient data enters the system, even in an MVP.
- You don't have to spend six figures to get started. Platforms like Specode let you build a working, HIPAA-compliant telehealth app in weeks with full code ownership, so you can validate fast and scale without vendor lock-in.
Why Peptide & Longevity Clinics Need a Custom Telemedicine Platform
If you run a peptide therapy or longevity clinic in 2026, you already know the landscape has shifted dramatically. The FDA's late-2023 decision to place 19 popular peptides on its Category 2 restricted list sent shockwaves through the industry, effectively banning compounding pharmacies from preparing compounds like BPC-157, TB-500, and CJC-1295. Then, in February 2026, HHS Secretary Kennedy announced that roughly 14 of those peptides would move back to Category 1, reopening legal access through licensed 503A compounding pharmacies with a physician's prescription.
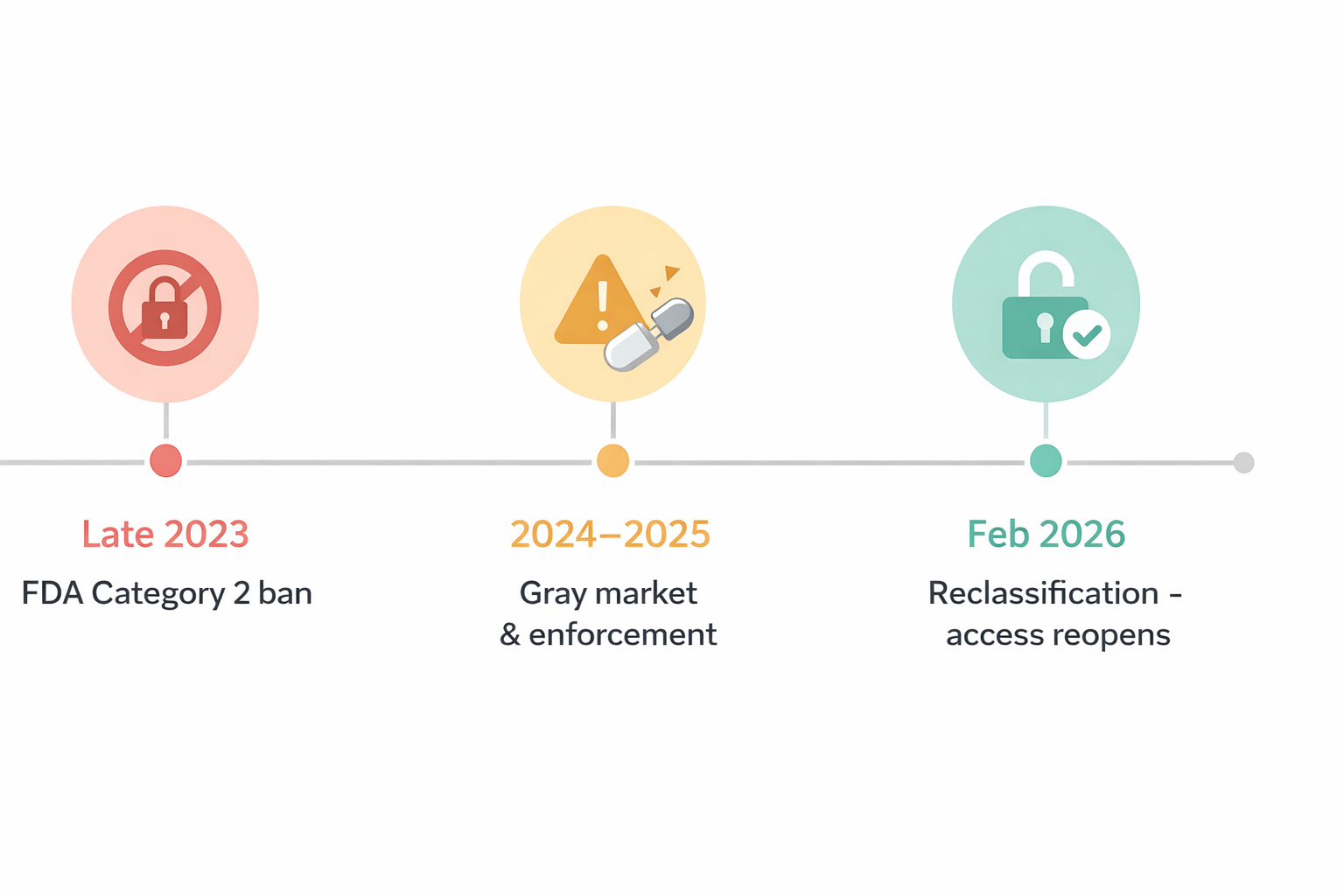
That regulatory whiplash created a very specific problem: clinics that relied on in-person visits and ad-hoc prescribing now need structured, compliant digital workflows to operate at scale. The old approach of seeing patients in-office and calling in prescriptions to a local compounder doesn't hold up when you're navigating:
- Multi-state prescribing rules and license tracking
- Mandatory diagnostic labs and synchronous video requirements for certain therapies
- The documentation burden that comes with off-label prescribing under evolving FDA guidance
Generic telehealth platforms like Doxy.me or off-the-shelf EHR systems weren't designed for this. They can handle a video call and a basic intake form, but they fall short on the workflows peptide and longevity clinics actually depend on:
- Long-form clinical intake forms with detailed medical history capture
- Risk stratification logic that flags patients for synchronous review
- Compounding pharmacy integration and e-prescribing via Surescripts
- AI patient education about dosing and safety profiles
Meanwhile, the market opportunity is real. Peptide-related search volume in the U.S. has reached over 10 million monthly searches, with longevity peptides specifically projected to cross 100K combined monthly searches by Q4 2026. The global longevity and anti-aging drugs market is expected to hit $21.47 billion this year alone. Med spas, wellness clinics, functional medicine practices, and compounding pharmacies are all racing to capture this demand through telemedicine. But the winners will be the ones who do it compliantly, with a purpose-built, HIPAA compliant telemedicine platform rather than duct-taped generic tools.
That's what this guide covers: how to build a digital health platform specifically designed for peptide therapy and longevity medicine, from clinical intake through e-prescribing and pharmacy fulfillment, with telehealth compliance baked in from day one.
What Is an Asynchronous Telemedicine Platform and Why It Works for Peptides
Most people think "telemedicine" means a video call with a doctor. That's synchronous telehealth, and it has its place. But when it comes to async telemedicine platform development, the more scalable model is store-and-forward telemedicine, where patients submit information on their own time and clinicians review it later.
The core flow looks like this:
- Patient intake. The patient completes a detailed medical intake form covering medical history, current medications, health goals, and contraindications.
- Provider review. A licensed clinician reviews the submission, orders labs if needed, and makes a prescribing decision without requiring a live appointment.
- Fulfillment. The prescription routes to a licensed 503A compounding pharmacy, which ships directly to the patient.
This model works particularly well for peptide clinics because most peptide protocols don't require a physical exam. The clinical decision hinges on lab work, medical history, and risk factors, all of which can be captured asynchronously. It also dramatically reduces clinician overhead: instead of blocking 15–30 minutes per patient for a video visit, providers can review charts in batches.
That said, async doesn't mean "never synchronous." A well-designed patient engagement platform triggers live video visits when they're clinically warranted, for example, when the intake reveals a complex medical history, flagged lab values, or a combination of medications that requires real-time discussion. Under the 2026 DEA/Ryan Haight telemedicine extension, certain therapies (particularly those involving controlled substances) still require a synchronous video consultation as part of the prescribing pathway. Your platform needs to handle both modes seamlessly.
Must-Have Features of a Peptide Telemedicine Platform
When scoping out peptide telemedicine app development, not every telehealth feature matters equally for this niche. Here's what a peptide and longevity clinic actually needs in a custom healthcare platform, organized by clinical workflow.
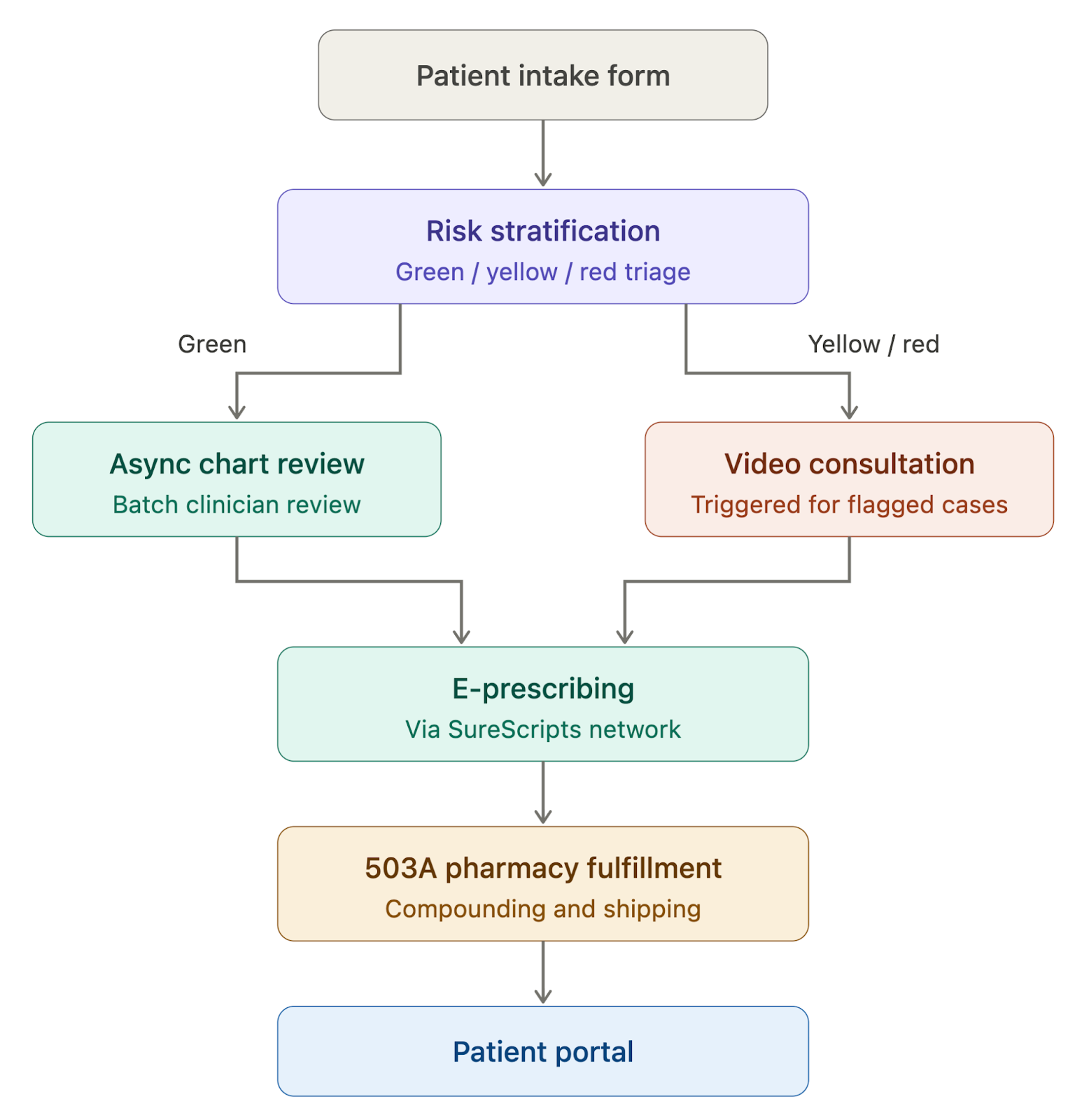
Patient Intake and Risk Stratification
Generic intake forms won't cut it. Peptide therapy requires a long-form patient intake questionnaire that captures detailed medical history, current supplements and medications, prior peptide use, contraindications, and specific health goals (recovery, metabolic optimization, immune support, longevity).
The real differentiator is AI-powered patient triage. Based on intake responses, the system should sort patients into tiers using a green, yellow, red alert system:
- Green — straightforward cases suitable for async chart review and prescribing
- Yellow — moderate complexity requiring additional labs or clinician attention before prescribing
- Red — flagged cases that trigger a mandatory synchronous video consultation
This triage logic keeps clinicians focused on the cases that need them most, while routine prescribing stays efficient.
AI-Powered Patient Education
Patients entering peptide therapy often have questions about dosing, administration (subcutaneous injection technique, reconstitution), cycling protocols, and safety profiles. A peptide education platform powered by AI can deliver personalized content based on the patient's prescribed protocol.
Important guardrail here: the AI should educate, not diagnose or prescribe. It can explain what BPC-157 is studied for, walk through proper injection technique, or clarify storage requirements. It should not make treatment recommendations or interpret individual lab results. Clear boundaries between education and clinical decision-making are both a requirement for telehealth compliance and a liability shield.
Async Chart Review and Clinician Dashboard
Clinicians need a purpose-built interface for reviewing patient submissions in batch, not a generic EHR inbox. Key elements:
- Patient summary cards with intake data, lab results, and risk tier at a glance
- Flagged items and alerts surfaced prominently
- One-click prescribing for straightforward green-tier cases
- Easy escalation to schedule a video visit for yellow/red cases
E-Prescribing and Pharmacy Integration
This is where many custom builds get complicated. To route prescriptions electronically to compounding pharmacies, your platform needs Surescripts integration, which requires your e-prescribing software vendor to be Surescripts-certified and, for controlled substances, to pass a DEA-required third-party audit.
For peptide clinics specifically, you'll also need:
- Multi-pharmacy partner routing (different 503A pharmacies may carry different compounds)
- Prescription management with tracking and patient notifications through fulfillment
- Support for multi-state prescriber management, since clinicians may hold licenses in multiple states and routing rules vary
Triggered Video Visits
When async review flags a patient for synchronous consultation, the platform should handle scheduling, video delivery, and documentation in one flow. You don't want clinicians switching between three tools to complete a flagged case. Options like Twilio, Daily.co, or CometChat (with its HIPAA-compliant plan) can power the video layer.
Secure Patient Portal and Messaging
Patients need a single place to view their treatment plan, track orders, message their provider, and access education content. HIPAA-compliant messaging (encrypted, access-controlled, audit-logged) is non-negotiable. This portal is also where you surface prescription status updates and lab requisition instructions.
Order Management and Fulfillment Tracking
Once a prescription is sent, both the clinic and the patient need visibility into the fulfillment pipeline: pharmacy received, compounding in progress, quality check passed, shipped, delivered. This is especially important for compounded peptides, which may have longer fulfillment timelines than standard prescriptions.
HIPAA Compliance and AI Guardrails
If you're building a telemedicine platform that handles peptide prescriptions, patient health data, and lab results, HIPAA compliance isn't a feature you bolt on later. It's an architectural decision you make on day one.
In practice, "HIPAA-compliant from day one" means your infrastructure, application logic, and third-party integrations all need to meet the Security Rule and Privacy Rule requirements before any real patient data enters the system. The core requirements include:
- Encryption at rest and in transit for all PHI (patient health information), including intake forms, lab results, prescriptions, and chat messages
- Role-based access controls so that clinicians, admins, and patients each see only what they're authorized to see
- Audit logging that tracks every access, modification, and transmission of PHI, with tamper-evident storage
- BAAs (Business Associate Agreements) with every service provider that touches PHI: your cloud host, database provider, email service, video calling platform, payment processor, and any analytics tools
This is where telemedicine software for compounding pharmacies gets especially tricky. Your platform doesn't just store patient data — it transmits prescriptions to external pharmacies, receives fulfillment updates, and may integrate with third-party lab ordering services. Each of those data flows needs its own HIPAA analysis and, in most cases, a signed BAA.
Multi-state telehealth adds another compliance layer. Prescribing rules, telemedicine practice standards, and even definitions of what constitutes a valid patient-provider relationship vary by state. Your platform needs to enforce the right rules based on the patient's location and the prescriber's license, not just your clinic's home state.
AI Guardrails for Medical Content
If your platform includes an AI-powered patient education module (and it should — see the features section above), you need explicit guardrails around what the AI can and cannot do.
The safe zone: delivering educational content about peptide mechanisms, explaining injection technique, summarizing published safety profiles, and answering general FAQs about protocols. The AI acts as a knowledgeable healthcare app development resource, not a clinician.
The red line: the AI must never diagnose, recommend specific peptides for a condition, interpret individual lab results, or adjust dosing. These are clinical decisions that require a licensed provider. Building these boundaries into the AI's system prompts and output filters isn't optional — it's how you avoid regulatory exposure and malpractice liability. Every AI interaction should also be logged for audit purposes.
E-Prescribing and Pharmacy Integration
E-prescribing is the technical backbone of any peptide telemedicine platform, and it's also where most teams underestimate the complexity. If you're planning to build a telemedicine platform from scratch, this is the section to study carefully. The same prescription routing logic also underpins standalone pharmacy app development — so if your clinic is evaluating a dedicated dispensing layer alongside your telehealth platform, that guide covers the full technical and compliance picture.
Surescripts Certification
To route prescriptions electronically to U.S. pharmacies, your platform's e-prescribing module must connect to the Surescripts network. This isn't a simple API integration. Your software vendor needs to achieve Surescripts certification, which involves conformance testing against NCPDP SCRIPT standards, production monitoring requirements, and ongoing compliance. For controlled substances (relevant if your clinic prescribes testosterone or other scheduled therapies alongside peptides), you'll also need EPCS (Electronic Prescribing for Controlled Substances) certification, which adds a DEA-mandated third-party security audit and two-factor authentication for prescribers.
Timeline reality check: Surescripts certification is not a weekend project. Plan for several months of development, testing, and review. Many teams opt to integrate with an already-certified e-prescribing platform (like RXNT, DoseSpot, or DrFirst) rather than pursuing certification independently.
Connecting to 503A Compounding Pharmacies
Standard retail pharmacies are well-connected to the Surescripts network. 503A compounding pharmacies, less so. Many compounders still rely on fax or direct portal integrations for receiving prescriptions. Your platform may need to support:
- Direct API integrations with your primary pharmacy partners
- Fallback to secure fax transmission where electronic routing isn't available
- Multi-pharmacy routing logic — different 503A partners may specialize in different peptide compounds, or your clinic may need regional pharmacy partners for faster shipping
Prescription Tracking and Patient Communication
Once a prescription leaves your platform, the patient shouldn't be left wondering what happened. Build a fulfillment tracking pipeline that captures key status updates — prescription received, compounding in progress, quality check passed, shipped, delivered — and surfaces them in the patient portal with push notifications or secure email alerts.
This is also where you'll want to learn how to create a telehealth app that feels polished rather than clinical. The patient experience around order tracking and communication is often what separates a platform that retains patients from one that loses them after the first prescription cycle.
Recommended Tech Stack
If you're working with a telemedicine app development company or a healthcare software development company to build a custom telehealth platform for med spas or peptide clinics, here's what a solid, modern tech stack looks like in 2026:
Frontend (patient app): React Native or Flutter for cross-platform mobile development. Both frameworks let you ship iOS and Android from a single codebase, cutting frontend costs by 30–40% compared to native development. For the clinician dashboard, a React or Next.js web app is the standard choice.
Backend: Node.js or Python, hosted on a HIPAA-compliant cloud provider (AWS, GCP, or Azure). All three offer BAAs, encryption at rest, and the compliance certifications (SOC 2, HITRUST) that procurement teams look for. Your backend handles authentication, role-based access, business logic for risk stratification, and API orchestration across integrations.
Database: PostgreSQL with encryption at rest, or a managed database service like AWS RDS or Google Cloud SQL. You'll need strict access controls and audit logging at the database layer, not just the application layer.
Video: Twilio, Daily.co, or CometChat (HIPAA plan) for triggered synchronous consultations. Pre-built SDKs save months compared to custom WebRTC implementations.
E-prescribing: Integrate with a Surescripts-certified platform (DoseSpot, DrFirst, RXNT) rather than pursuing certification independently. This is the single biggest time-saver in the entire stack.
AI layer: LLM integration for AI patient education, intake summarization, and clinical workflow automation. The AI handles content delivery and data structuring, not clinical decisions.
Email: A HIPAA-compliant transactional email provider (Mailgun's HIPAA plan, Paubox) for appointment reminders, prescription notifications, and secure communications.
This is a proven, portable stack. Every component is interchangeable, nothing locks you into a single vendor, and you can self-host the entire thing if you outgrow managed services. It's also the kind of stack that med spa software vendors and weight loss platform operators increasingly expect when evaluating telemedicine infrastructure. But it takes 6–10 months and $80K–$150K+ to build out properly, which brings us to timelines and costs.
How to Scale Beyond MVP: From 350 to 30,000 Patients
The temptation when you build a telemedicine platform for weight loss clinics, peptide practices, or longevity medicine is to over-engineer the MVP. Don't. Your first telemedicine MVP needs to serve your initial patient base reliably, not handle 30,000 concurrent users.
Start with the core loop: intake → risk stratification → async chart review → prescribing → pharmacy fulfillment → patient portal. Get this workflow airtight for your first 200–500 patients before layering on advanced features.
When you're ready to scale, focus on these areas:
New treatment protocols. Your platform's data model should accommodate new peptide categories, dosing protocols, and treatment plans without requiring a code rewrite. Build protocol management as a configurable layer, not hardcoded logic.
Multi-clinic and white-label architecture. If you plan to license your platform to other clinics or operate multiple brands, design for multi-tenancy early. Retrofitting tenant isolation into a single-tenant app is painful and expensive.
Analytics and outcomes tracking. Longevity medicine patients expect data. Build dashboards that track biomarkers over time, correlate treatment protocols with outcomes, and give clinicians aggregate insights across their patient panel. This data also becomes your strongest marketing asset: real outcomes from real patients.
Remote patient monitoring. Integrating wearables and connected devices (CGMs, HRV monitors) opens up a remote patient monitoring revenue stream and strengthens clinical decision-making with continuous data rather than periodic snapshots.
Telemedicine Platform Development Cost and Timeline
Let's talk real numbers. Telehealth MVP development costs vary widely depending on scope, but for a peptide-focused telemedicine platform with the features described in this guide, here's what to expect in terms of telehealth platform cost:
These ranges assume a U.S.-based or blended development team working with HIPAA-compliant infrastructure from day one. Offshore-only teams may quote lower, but healthcare compliance expertise is not where you want to cut corners.
Beyond the initial build, budget for ongoing costs:
- Cloud hosting and infrastructure: $1,000–$5,000/month depending on scale
- Surescripts/e-prescribing platform fees: varies by vendor and volume
- Maintenance, security patches, and compliance updates: 15–20% of initial build cost per year
- Third-party API fees (video, email, AI): $500–$3,000/month
The biggest cost lever is how you approach the build. Going fully custom with a traditional development team means maximum control but also maximum spend and timeline. There's a faster path, which we'll cover next.
How Specode Can Help
Everything above describes the traditional route: assemble a dev team, choose a stack, spend months on compliance architecture, and budget six figures before your first patient logs in. It works, but it's slow and expensive.
Specode is an AI-powered healthcare application builder designed specifically for this problem. Instead of hiring a full development team, you describe what you want in plain English, and Specode's AI assistant builds it using a HIPAA-ready foundation. Auth, encryption, secure data access patterns, and audit-friendly workflows are built in from day one, not bolted on after the fact.
Here's what that means in practice for a peptide or longevity clinic:
- You define your own workflows. Specode isn't a template system. You describe your intake flow, risk stratification logic, clinician dashboard, and patient portal, and the AI builds it to your spec. Need a green/yellow/red triage system? Describe it. Need custom fields for peptide protocol tracking? Describe those too.
- Production deployment with HIPAA infrastructure included. On the Pro plan ($1,000/month), you get production hosting with a backend BAA included, no need to negotiate your own hosting agreements or set up separate HIPAA-compliant cloud accounts.
- Full code ownership. Unlike no-code platforms that lock you in, Specode gives you 100% of the source code. Export it anytime, deploy it anywhere, hand it off to your own dev team if you outgrow the platform. The tech stack underneath (React frontend, Convex backend) is modern and portable.
- Built-in HIPAA compliance scanning. Specode includes a Compliance Center with a multi-agent HIPAA scanner that audits your codebase for potential violations. Run it on demand, fix flagged issues through the AI chat, and re-scan to confirm.
- Expert support from healthcare tech veterans. Pro and Custom plans include PM consultation, weekly team support, and unblocking sessions. You're not debugging compliance issues alone.
A basic telehealth app can be up and running in 1–2 weeks rather than 3–5 months. And because you own the code, you're not trading speed for flexibility. If you need custom integrations with 503A pharmacy partners, CometChat for video visits, or Stripe for payment processing, the AI builds those in.
For clinics that need more hands-on help, the Custom plan (starting at $5,000/month) includes managed coding, dedicated team support, and custom AI agents tailored to your specific clinical workflows.
Ready to build? Start building on Specode or book a discovery call to talk through your longevity clinic telemedicine software with the team.
Frequently asked questions
A peptide-focused platform needs long-form clinical intake with medical history capture, automated risk stratification (green/yellow/red triage), async chart review for efficient prescribing, e-prescribing integration with 503A compounding pharmacies, and multi-state prescriber license management. Generic telehealth tools handle video calls and basic scheduling but lack these niche-specific workflows.
Start with HIPAA-compliant infrastructure (encrypted databases, access controls, audit logging) and sign BAAs with every service provider that touches patient data. Even in an MVP, never store PHI in non-compliant environments. Platforms like Specode can shorten that path by providing a HIPAA-ready foundation for production deployments, but you still need to configure the right vendors, data flows, and BAAs for your specific setup.
Yes, though the integration method varies. Some 503A pharmacies support direct API connections; others still operate via secure fax or web portals. A well-designed platform supports multiple routing methods and can manage several pharmacy partners simultaneously for different compound types.
With a traditional dev team, expect 3–5 months for a basic MVP and 6–12 months for a full-featured platform. Using an AI-powered builder like Specode, a basic telehealth app can be functional in 1–2 weeks, with more complex features added iteratively.
Custom development typically ranges from $40,000–$70,000 for a basic MVP to $150,000–$300,000+ for an enterprise platform. Specode's Pro plan at $1,000/month offers a significantly faster and more affordable path, with full code ownership so you can migrate to self-hosted infrastructure as you scale.
AI can deliver personalized educational content about peptide mechanisms, injection techniques, storage requirements, and protocol FAQs. The key guardrail: AI educates but never diagnoses, recommends treatments, or interprets individual lab results. Those decisions stay with licensed clinicians.